Swift Action Results in Change of Telehealth Regulations
- 8 April 2020
- Blog
eClinicalWorks

Pandemic spurs action in Congress, leads to waivers
Extraordinary times demand extraordinary responses. The coronavirus pandemic has sparked quick action from Congress, providing monetary assistance to the healthcare community as well as easing regulations.
That assistance includes funding for supplies such as masks, ventilators, and testing kits, and a less tangible but equally important relief — flexibility in the rules that govern how medicine gets done.
Congress moves quickly
While most legislation can take months to become law, the $8.3 billion Coronavirus Preparedness and Response Supplemental Appropriations Act was introduced on March 4 and signed into law by President Trump on March 6.
The legislation includes waivers that allow providers — including doctors, nurses, psychologists, and social workers — to use telehealth technologies to provide preventive screenings, routine office visits, and mental health counseling to Medicare beneficiaries.
Medicare summaries and in-depth guidance
- For an overview of the new rules, consult this Medicare telehealth fact sheet from the Centers for Medicare & Medicaid Services.
- Practices with specific questions or seeking in-depth guidance can refer to the Coronavirus Waivers & Flexibilities list from CMS.
- The Centers for Disease Control and Prevention have issued these coronavirus guidelines for anyone seeking information about risk and symptoms.
A comprehensive telehealth solution
With new flexibility governing telehealth, practices in search of solutions should remember two key points:
- Your practice should look for a proven, HIPAA-compliant solution that fully protects your patients’ personal information, works with your EHR, and can be used with any browser and on any device.
- You want more than a way to talk with patients remotely. Choose a vendor with a comprehensive solution that allows complete documentation and includes tools for analytics, outreach, and follow-up care.
healow Telehealth Solutions from eClinicalWorks meets all these criteria and more. Our stand-alone telehealth solutions are the secure, affordable choice for your practice and can be up and running in just days.
Private payers: Policies may vary
It is important for providers to understand that the new flexibility in providing services — including telehealth services — is not the whole story. The guidelines above apply only to Medicare beneficiaries. Extending care to patients covered by private insurers may be governed by other rules and policies that can vary from state to state and from one insurer to the next.
As outlined in this article from the Kaiser Family Foundation, many states are now requiring private insurers to cover the costs of testing and treatment related to COVID-19. However, because the rules remain a mix of requirements and advisories, practices should double-check coverage for services to patients not covered by Medicare.
Related Post

- 9 January 2025
- Blog
Unveiling Trends Set to Transform Healthcare in 2025

- 15 February 2024
- Blog
AI Medical Scribes in Remote Healthcare Services

- 7 November 2023
- Blog
Embracing Technology for Startup Weight Loss and Medical Spa Clinics

- 27 September 2022
- Blog
Back to School — for Your Practice, Too!

- 21 June 2022
- Blog
Dermatology Made Easier This Summer

- 25 March 2022
- Blog
HIMSS22 Outlines Opportunities in Healthcare

- 17 February 2022
- Blog
Defense Matters: Keeping Remote Medicine Safe

- 1 February 2022
- Blog
One Key for 2022: Staying Focused on Patients

- 28 January 2022
- Blog
4 Patient Engagement Solutions to Help Patients and Practices in 2022

- 25 January 2022
- Blog
The Right Tools During Challenging Times

- 19 January 2022
- Blog
Healthcare 2022: Regulatory Trends to Look for in the Year Ahead

- 18 November 2021
- Blog
Remaining Vigilant in the Lung Cancer Fight

- 4 November 2021
- Blog
Telehealth Is Long-Established Science Fact

- 2 September 2021
- Blog
It’s Time for a Better Check-in Solution

- 12 August 2021
- Blog
Using hello2healow for Patient Outreach in Florida

- 27 May 2021
- Blog
When Neurological Care Cannot Wait

- 20 May 2021
- Blog
Solutions for Allergy Testing, Tracking, and Treatment

- 16 March 2021
- Blog
A Partner for Reinventing Your Practice

- 2 March 2021
- Blog
What it Takes to Better Know Your Patients

- 29 January 2021
- Blog
Putting the Pieces Together for Quality Healthcare

- 30 December 2020
- Blog
2020 eClinicalWorks Year in Review

- 22 December 2020
- Blog
Thirlby Clinic: Using Telehealth and CCM for Better Disease Management

- 15 December 2020
- Blog
A Challenging Year Is Ending — New Opportunities Ahead

- 10 December 2020
- Blog
How a Practice Found Success With Telehealth & Contactless Check-In

- 24 November 2020
- Blog
The Continuing Influence of Telehealth

- 19 November 2020
- Blog
Meeting the Demand for Behavioral Health Services

- 12 November 2020
- Blog
Reinventing Healthcare for a Brighter Future

- 6 November 2020
- Blog
How Little River Medical Center Thrived During the Pandemic

- 19 October 2020
- Blog
How Telehealth, CCM, and Contactless Check-In Revitalized a Practice in Need

- 15 October 2020
- Blog
Targeting Behavioral Health, Remote Care & More

- 30 September 2020
- Blog
Surviving COVID-19: Telehealth and Beyond
- 21 September 2020
- Blog
3 Important healow TeleVisits Features

- 9 September 2020
- Blog
It’s Your Practice — Dream Big!

- 1 September 2020
- Blog
Back to the Basics During the COVID-19 Era

- 28 August 2020
- Blog
How the Patient Portal Is Making a Difference for a Pediatric Practice

- 24 July 2020
- Blog
Pushing Boundaries, Reaching New Horizons

- 17 July 2020
- Blog
How to Keep Your Patients & Staff Safe During COVID-19

- 1 July 2020
- Blog
How to Digitize Your Front Office

- 29 June 2020
- Blog
The Telehealth Revolution Continues

- 24 June 2020
- Blog
How Advocare Put healow TeleVisits™ to Work
- 17 June 2020
- Blog
How Telehealth Is Connecting Patients & Providers

- 12 June 2020
- Blog
Finding a New Normal: The Patient Experience

- 10 June 2020
- Blog
Minding Mental Health During COVID-19

- 3 June 2020
- Blog
Expanding the Range of Specialty Care

- 1 June 2020
- Blog
Reinventing Your Practice

- 29 May 2020
- Blog
What Telehealth Could Mean for Practices Today

- 27 May 2020
- Blog
Resourceful Action During Extreme Times

- 21 May 2020
- Blog
Like Telehealth? There’s More!

- 19 May 2020
- Blog
The Numbers Behind TeleVisits

- 16 May 2020
- Blog
What Telehealth Can Do for Specialty Practices

- 13 May 2020
- Blog
Routine Care During Nonroutine Times

- 12 May 2020
- Blog
How Telehealth Will Make The 21st Century Ours

- 8 May 2020
- Blog
Seeing Medicine in a New Light

- 7 May 2020
- Blog
Telehealth: Healing Action at a Distance

- 5 May 2020
- Blog
3 Patient Stories of TeleVisits in Action

- 1 May 2020
- Blog
Sustaining Medical Practice During COVID-19
- 29 April 2020
- Blog
The Evolution and Importance of Telehealth

- 27 April 2020
- Blog
Deriving Greater Value from Telehealth

- 24 April 2020
- Blog
3 Practices Finding Success With Telehealth

- 22 April 2020
- Blog
How Innovation Fueled the Rise of Telehealth

- 20 April 2020
- Blog
Why You Should Activate Telehealth Today

- 17 April 2020
- Blog
3 Practices Using Telehealth to Improve Patient Care

- 15 April 2020
- Blog
Shift in the Medical Mindset

- 13 April 2020
- Blog
How Telehealth Kept a Patient Out of the ER

- 10 April 2020
- Blog
Speeding Toward a New Healthcare Paradigm

- 9 April 2020
- Blog
How Dallas Renal Group is Providing Care While Social Distancing
- 7 April 2020
- Blog
How Central Ohio Primary Care Physicians is Reducing ER Visits

- 6 April 2020
- Blog
Securing Access to Care During a Pandemic

- 3 April 2020
- Blog
How Telehealth is Keeping Patients Safe at Trusted Doctors

- 2 April 2020
- Blog
Flattening the Curve With Telehealth

- 1 April 2020
- Blog
How First Choice Neurology Transformed Their Practice With Telehealth

- 31 March 2020
- Blog
Telehealth and Mental Health in a Time of Crisis

- 27 March 2020
- Blog
How SG Pediatrics are Using TeleVisits to Help Patients

- 26 March 2020
- Blog
The eClinicalWorks Telehealth Advantage

- 25 March 2020
- Blog
How Televisits Have Transformed Comprehensive Sleep Center

- 24 March 2020
- Blog
Telehealth: Helping Throughout History

- 23 March 2020
- Blog
How healow TeleVisits Can Help During a Health Crisis

- 20 March 2020
- Blog
healow TeleVisits: How Fast Deployment Helps
- 11 March 2020
- Blog
Expanding Access to Care With healow TeleVisits

- 17 January 2020
- Blog
Teledentistry: Expanding Access to Dental Care
- 8 January 2020
- Blog
The State of Telehealth in 2020

- 14 August 2019
- Blog
Patient-Centered Care: How the Approach Can Improve Healthcare

- 5 June 2019
- Blog
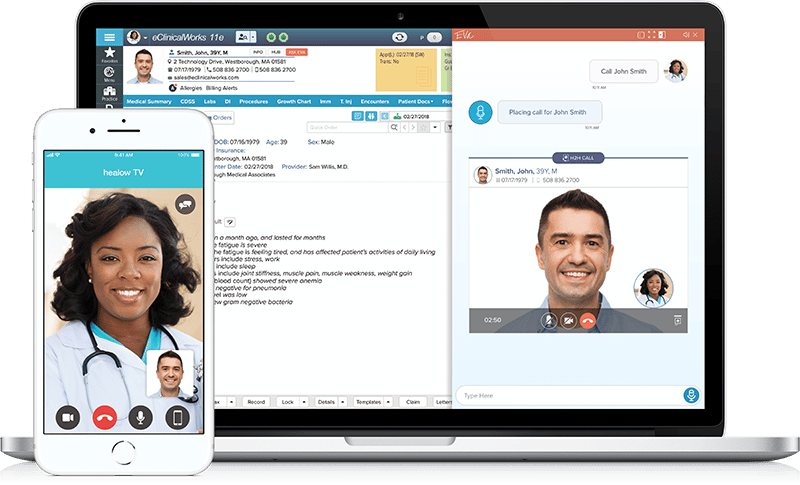
3 Ways That Telehealth Is Improving Healthcare
- 9 January 2019
- Blog
Telehealth – Rural Health Center
- 1 November 2018
- Blog
Three Ways Telemedicine Improves Care for Providers and Patients

- 15 October 2018
- Blog
How telehealth helps to improve compliance among ADHD patients

- 7 October 2018
- Blog
Powering Through on Game Day!

- 6 October 2018
- Blog
Making Connections on Saturday

- 30 May 2018
- Blog
ADHD and Telemedicine: A Natural Fit
- 20 March 2015
- Blog
The Next Phase of Innovation in Healthcare
- 20 March 2015
- Blog








